Charcot-Marie-Tooth Disease
What is Charcot-Marie-Tooth disease?
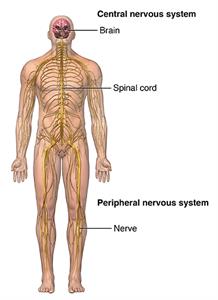
Charcot-Marie-Tooth (CMT) disease is an inherited nerve problem. It causes abnormalities in the nerves that supply your feet, legs, hands, and arms. It affects both your motor and sensory nerves. Motor nerves carry signals from your brain to your muscles, telling them to move. Sensory nerves carry sensations, such as heat, cold, and pain back to your brain. CMT is considered a peripheral neuropathy because it affects nerves outside of your brain and spinal cord.
This disease is named after the 3 doctors who first described the disease in 1886. It is one of the most common types of inherited nerve diseases.
What causes Charcot-Marie-Tooth disease?
CMT is almost always caused by a gene problem inherited from one or both parents. The genetic information that one or both of your parents passes on to you determines the type of gene change (mutation) you have. This gene mutation determines what symptoms you have and how old you are when they start. There are more than 30 known genetic causes of CMT. The exact cause of many more forms has yet to be identified.
Some genetic problems affect the axon. This is the part of the nerve that sends signals to other nerves. Other genetic problems affect the protective lining around the axon (myelin sheath). Either type of problem can lead to long-term damage of the nerve and affect its ability to send signals.
What are the symptoms of Charcot-Marie-Tooth disease?
CMT symptoms may vary from person to person, though they usually start in your feet and legs. Over time, the disease may also affect your hands and arms. Symptoms usually first appear in teens and young adults.
Common symptoms include:
- Weakness of your foot and lower leg muscles
- Foot deformities, including a high arch and bent toes (hammer toes)
- Difficulty lifting your foot while walking (foot drop)
- Loss of muscle around your hands and feet
- Numbness, tingling, burning, or loss of temperature sensation in your hands and feet
- Discomfort or pain in your hands and feet
- Abnormal curvature of the spine (scoliosis)
How is Charcot-Marie-Tooth disease diagnosed?
A specialist called a neurologist may diagnose CMT after doing a complete nervous system exam and asking about your family history. Tests that help make the diagnosis include:
- A blood test to look for genetic problems
- Nerve conduction studies to measure the strength and speed of electrical signals passing through your nerves
- Electromyography to measure how well your nerves communicate with your muscles
-
Nerve biopsy. This means taking a small piece of a nerve and looking at it under a microscope. This is often done if blood work can't find the genetic cause of the symptoms
If you have no family history of this disease, your healthcare provider may consider looking for other causes of your symptoms.
How is Charcot-Marie-Tooth disease treated?
There is no cure for CMT. But these treatments can help:
- Physical therapy to strengthen and stretch your muscles. This may help prevent or delay disability caused by weakness and deformity.
- Occupational therapy to help with your daily activities. This includes using special devices like rubber grips, or changing from buttons and zippers to Velcro.
- Orthopedic devices such as ankle braces, high-top boots, and thumb splints.
- Pain medicines if needed.
- Surgery for severe deformities of the feet, spine, or other joints.
What are possible complications of Charcot-Marie-Tooth disease?
CMT is not a fatal disease. Most people with it live to a normal age and remain active. In rare cases, it may affect the muscles you need to breathe. Because this can be especially dangerous at night, you may need a nighttime breathing assistive device.
More common complications are:
- Injuries from falls
- Worsening of the disease that certain medicines can cause
- Injuries or infections of the feet that go unnoticed because of lack of pain and temperature sensation
Living with Charcot-Marie-Tooth disease
It's very important to learn as much as you can about your disease. Work closely with your neurologist. Genetic counseling may be important for family planning. Other ways to manage your disease include:
- Getting regular low-impact aerobic exercise
- Not drinking alcohol except in moderation
- Eating a healthy diet and staying at a healthy weight
- Checking your feet regularly for any injury or infection
- Checking with your healthcare provider before taking any new medicines. Certain medicines can make your symptoms worse.
When should I call my healthcare provider?
Call your healthcare provider if you have:
- Any new or worsening symptoms
- Signs of foot injury or infection
- Trouble breathing
Key points Charcot-Marie-Tooth disease
- Charcot-Marie-Tooth disease is an inherited disorder. It affects the nerves supplying the feet, legs, hands, and arms. It's caused by gene defects that are nearly always inherited from a person's parents.
- Symptoms often begin in the teen or early adult years. They can include weakness in the feet and legs and foot deformities. Over time, the hands and arms might be affected as well.
- Charcot-Marie-Tooth can't be cured at this time. But treatments such as physical and occupational therapy can often be very helpful. Most people with this condition live to a normal age and remain active.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
- Know the reason for your visit and what you want to happen.
- Before your visit, write down questions you want answered.
- Bring someone with you to help you ask questions and remember what your provider tells you.
- At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
- Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
- Ask if your condition can be treated in other ways.
- Know why a test or procedure is recommended and what the results could mean.
- Know what to expect if you do not take the medicine or have the test or procedure.
- If you have a follow-up appointment, write down the date, time, and purpose for that visit.
- Know how you can contact your provider if you have questions.
Get the care you need from world-class medical providers working with advanced technology.
Cedars-Sinai has a range of comprehensive treatment options.


