Research Areas
Hormonal Contraceptives Reduce Ligament Laxity and Protect Against Injuries in Female Athletes
Female athletes have a 3 to 9 times greater risk of rupturing their anterior cruciate ligament (ACL) compared to similarly trained males playing the same sport and the same level. Female sex hormones may play a role in altering the ability of our ligaments to resist mechanical stress. Our data suggests hormonal contraceptives (HC) reduce fluctuations in female reproductive hormones, decrease ligament laxity, and reduce the risk of injury in high-level female athletes.

Biomechanical Comparison of Achilles Tendon Pullout Strength Following Midline Tendon-splitting and Endoscopic Approaches for Calcaneoplasty
Haglund's syndrome occurs when there's an enlargement of the bony section of the heel, which causes irritation to the area's soft tissue. If nonsurgical methods fail to provide relief, surgical removal of the bone, or calcaneoplasty, can be performed to manage Haglund's syndrome. Calcaneoplasty can either be an open procedure (i.d., midline tendon splitting) or it can be performed endoscopically. To confirm previous studies suggesting that the endoscopic technique provides quicker return to activity and superior outcomes, a biomechanical comparison study was performed. By quantifying and comparing Achilles tendon pullout strength after both calcaneoplasty methods using human cadaveric specimens, results confirmed that endoscopic calcaneoplasty had more than three times greater pullout strength.

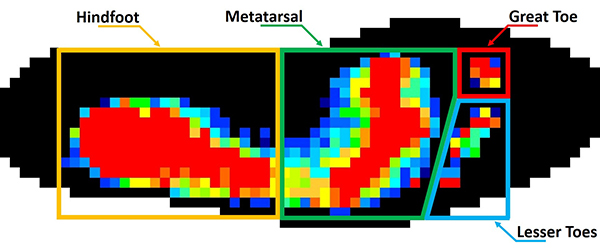
Biomechanical Impact of FHL Tendon Harvest on Forefoot and Great Toe Push-off Strength and its Correlation to Knot of Henry Crossover Variation
Some patients undergoing reconstructive Achilles tendon surgery, where the flexor hallucis longus (FHL) tendon is used for tendon transfers, complain of great toe weakness and loss of push-off strength. A biomechanical human cadaveric study was performed to quantify strength and determine if the crossover patterns at the Knot of Henry (KOH) lead to forefoot weakness. Simulated FHL harvest resulted in decreased great toe flexion pressure and total forefront flexion pressure in all specimens, with no significant differences between KOH crossover patterns.
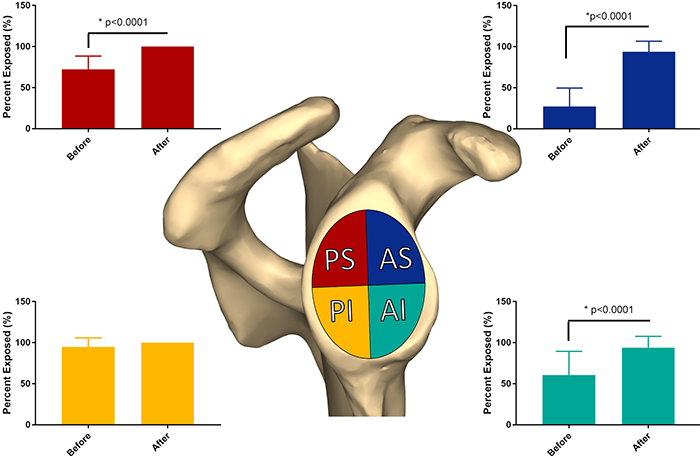
Infraspinatus Tenotomy Improves Glenoid Visualization with the Modified Judet Approach
The modified Judet approach (MJA) is a surgical procedure for scapula fractures that lessens soft tissue trauma; however, it limits exposure of the glenoid socket that holds the humerus. The purpose of this study was to determine if adding an infraspinatus tenotomy—surgical cutting of the triangular muscle of the scapula for shoulder joint motion and stability—to the MJA improves glenoid visualization. The MJA was performed on human cadaveric shoulders to determine the percentage of glenoid visualized before and after adding a tenotomy. Results demonstrate that adding an infraspinatus tenotomy to the MJA significantly increased visualization of the glenoid area.
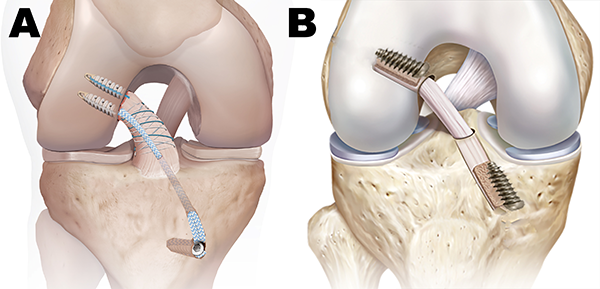
Anterior Cruciate Ligament Repair Versus Reconstruction: A Kinematic Analysis
After injury, two procedures to restore the anterior cruciate ligament (ACL)—a major ligament connecting the thigh bone to the shin bone—are ACL repair and ACL reconstruction. This study compares the biomechanical properties after each procedure by analyzing knee range of movement in paired human cadaveric knees. ACL repair and ACL reconstruction both comparably restored knee anterior tibial translation; although, knee motion after ACL repair was closer to presurgical (intact) knee motion.
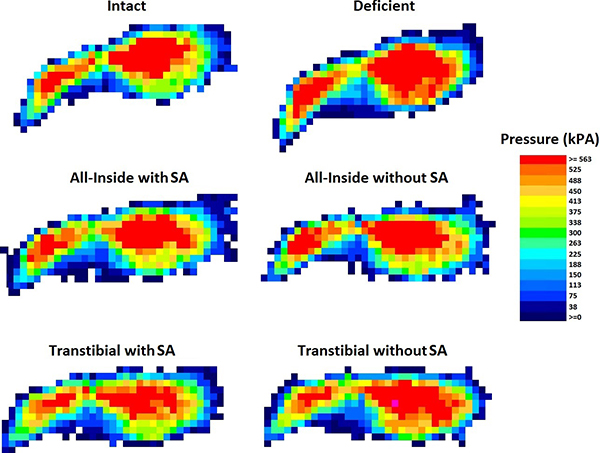
Biomechanical Evaluation of PCL Reconstruction with Suture Augmentation
The posterior cruciate ligament (PCL) in the knee also connects the thigh bone to the shin bone. Two techniques to repair injuries to the PCL are the all-inside and transtibial single bundle PCL reconstructions. This study compares motion and patellofemoral contact pressures after each procedure and determines if suture augmentation additionally improves biomechanics. Human cadaveric knees were tested with a posterior drawer force, and varus, valgus, internal and external moments at varying degrees of flexion. Both all-inside and transtibial single bundle PCL reconstructions reduce posterior translation, and suture augmentation with both techniques provides additional anterior-posterior stability.
A Comparison of Three Fixation Strategies in the Treatment of Neer Type IIB Distal Clavicle Fractures
Unstable Neer type IIB (NT2B) distal clavicle fractures have high nonunion rates due to the rupture of coracoclavicular ligaments. This study compares the multi-planar stability of NT2B clavicle fractures created in human cadaveric specimens that were repaired with either hook plating (HP), superior plating with suture augmentation (SPSA) or dual orthogonal mini-fragment plating (DP). Specimens were loaded while displacement was recorded in three planes of motion: anteroposterior, superior-inferior and axial rotation. Clavicles fixed with a DP had improved stability against anterior displacement during anteroposterior and superior-inferior loading than HP and SPSA; although, there was no significant difference in superior stability, axial rotation stability, stiffness or load to failure.

Extensor Tendon Transfers for Treatment of Foot Drop in Charcot-Marie-Tooth Disease: A Biomechanical Evaluation
One symptom of Charcot-Marie-Tooth disease—an inherited, peripheral neuropathy disorder—is foot drop, a weakness of the ankle and toe dorsiflexion. Due to weakness of the tibialis anterior muscle, the long toe extensors may be used as secondary dorsiflexors, which leads to clawing of the toes. This study transects human cadaveric specimens midtibia and isolates and connects tendons to extensor hallucis longus and extensor digitorum longus muscles to minimize claw toe deformity. Results showed that transfer of the long toe extensors to either the metatarsals or cuneiforms significantly increased ankle dorsiflexion compared to the intact state.
Contact the Metzger Lab
8700 Beverly Blvd.
Davis Building, Room 6006
Los Angeles, CA 90048