Research Areas
Immune Responses in Inflammatory Bowel Disease
The Michelsen Laboratory is particularly interested in the role of the innate immune system in the development of inflammatory bowel diseases (IBD). Recent reports have shown that genetic variations in the gene encoding for a tumor necrosis factor family member called tumor necrosis factor-like cytokine 1A (TL1A) confer susceptibility to IBD.
TL1A is a protein that is upregulated during chronic intestinal inflammation in IBD, particularly in inflamed areas of the intestine. TL1A is produced by antigen-presenting cells upon encounter with enteric bacteria or immune complexes. TL1A is a proinflammatory cytokine that exerts its effects on several different cell types, including T helper cells, innate lymphoid cells and fibroblasts, thereby worsening intestinal inflammation and fibrosis (Figure 1).
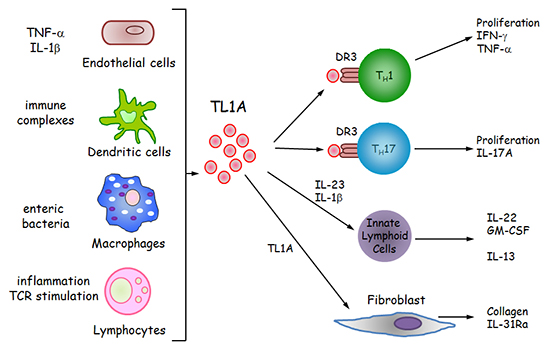
Figure 1: TL1A is induced by several different cell types in response to immune complexes, enteric bacteria and inflammatory stimuli. TL1A exerts its effect on T helper cells, innate lymphoid cells and fibroblasts by increasing their production of proinflammatory mediations leading to disease exacerbation.
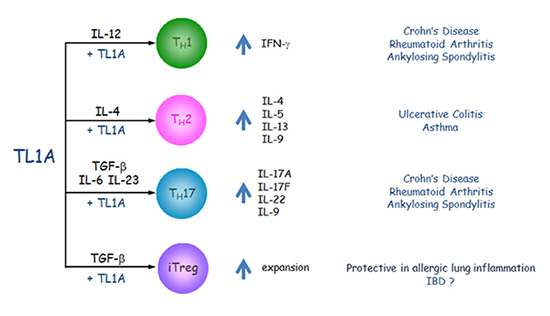
Figure 2: Effects of TL1A on different T helper cell subsets and their involvement in diseases. TL1A in combination with other cytokines increases the production of proinflammatory mediators that lead to exacerbation of diseases such as inflammatory bowel diseases (ulcerative colitis, Crohn's disease), rheumatoid arthritis, asthma and ankylosing spondylitis.
Genotype-Phenotype Correlation in Patients with IBD
Genome-wide association studies have identified more than 160 genetic loci associated with the susceptibility to IBD. Many of these loci are shared with other immune-related diseases such as rheumatoid arthritis, ankylosing spondylitis, lupus and leprosy. However, the functional consequences for genetic variations in these susceptibility loci in patients with IBD are largely unknown. We are interested in determining the functional consequences of genetics variations in immune-related genes by analyzing patients carrying risk or protective variations for these genes.
Understanding the molecular mechanisms that lead to the development of inflammatory bowel diseases will be important for the development of novel therapeutics for IBD.
Contact the Michelsen Lab
8700 Beverly Blvd.
Davis Research Building, Room 4058
Los Angeles, CA 90048